Information for Caregivers
Key points
- Your child will recover from the surgery for 5-7 days.
- Some children with a trach tube may eventually be able to use their voice and/or make sounds. Some can eat and drink by mouth.
- We train 2 caregivers to care for your child’s trach tube at home.
What is a tracheostomy (trach)?
A tracheostomy is an opening in the throat that goes into the windpipe (trachea). A tracheostomy tube is placed in the opening to help your child breathe.
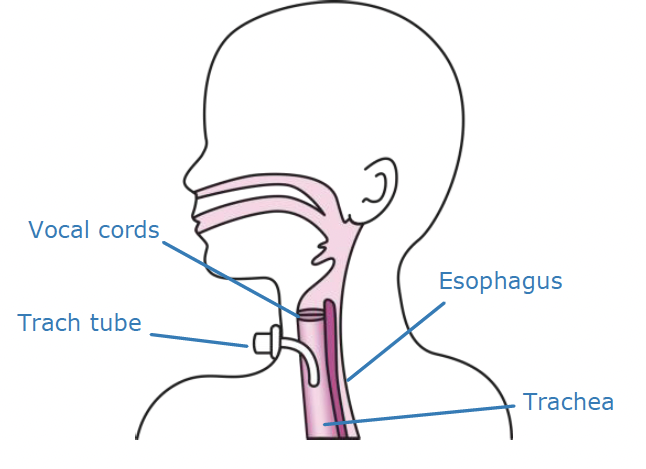
Why might my child need a trach tube?
There are many reasons why people may need a trach tube. Some reasons are:
- Airway issues
- Chronic lung disease
- Frequent lung infections
How does a trach help?
The benefits are specific to each child. In general, the trach helps by:
- Replacing the need for a breathing tube, which can irritate the vocal cords
- Relieving an upper airway obstruction
- Making it easier to remove secretions
- Allowing doctors to lower or take your child off the sedation being used to keep the breathing tube safely in place while your child needs to be on a ventilator
- Helping with rehabilitation (your child’s ability to get better and be more active)
Who performs the surgery and what should I expect?
- An airway surgeon called an otolaryngologist (ORL) performs the procedure.
- We will talk to you about the risks of procedure and get your permission (consent) to do the surgery.
- The surgery takes about 1 hour.
- Your child will recover for 5-7 days. During this time, it’s important for your child to be as still as possible to help them heal.
- Your child may need sedation and/or other medications to help keep them still.
- The ORL team will come to your child’s bedside every day during their recovery to check the dressing and to look at the surgical site.
- After 5-7 days, ORL will do the first trach tube change at the bedside, if your child is stable.
- This involves removing the trach tube and replacing it with a new trach tube.
- If there are no issues with the first trach change, the care of the trach is passed onto the ICU team and nursing staff.
Pediatric cuffed trach tube with a flextend
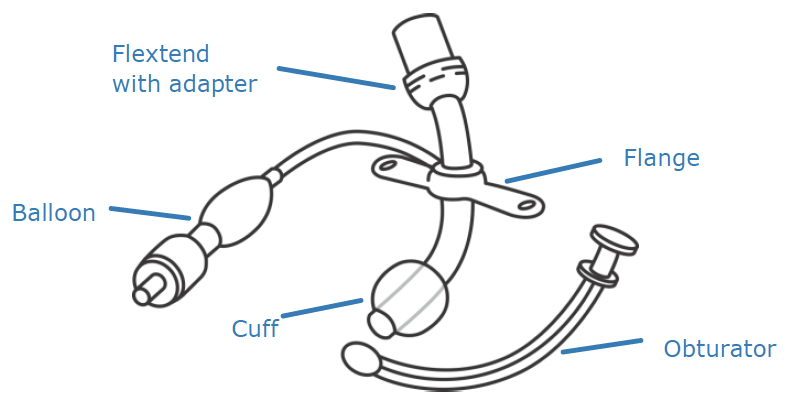
Pediatric cuffed trach and adult cuffed trach tube
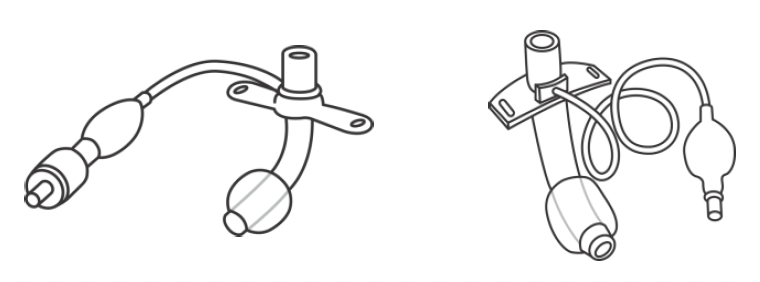
How do I learn how to take care of my child’s trach?
We train 2 caregivers to care for your child’s trach tube at home. After the first trach change, nurses and respiratory therapists will begin to teach you to care for the trach, if your child is stable.
You will learn about:
- Site care
- Go-bag
- Open and closed (if applicable) suctioning
- Trach emergencies and CPR
- Use of the self-inflating bag
- Speaking valve (if applicable)
- How to change the trach
- Safely traveling
- Types and importance of humidification
- Trach/ventilator (if applicable) emergency simulation
Who is on my child’s care team?
The Tracheostomy Team includes otolaryngologists, nurses, respiratory therapists, speech and language pathologists, case managers, occupational therapists, physical therapists, the feeding team and Child Life specialists.
How will my child communicate with a trach?
- People with a trach communicate in many different ways. This includes speech, sign language, nonverbal communication (gestures, facial expressions, head nods), writing/typing and augmentative and alternative communication (AAC) strategies.
- Some children with a trach tube can use their voice and/or make sounds.
- Some children can use a small cap-like device that fits on the outside of the trach tube. It’s called a speaking valve.
- Many children benefit from use of additional strategies to support their communication development and expressive language.
- A speech-language pathologist will help you and your child find the best way for them to communicate and express themselves.
- Your child’s medical team, respiratory therapist and speech-language pathologist can help you learn more about your child’s ability to use their voice with a trach.
Will my child be able to eat and drink by mouth with a trach tube?
- Some children with a trach tube can eat and drink by mouth.
- Your child will have a feeding evaluation and/or a modified barium swallow study to see if they can eat or drink.
- Some children need a feeding tube (nasogastric tube, gastrostomy tube or gastrostomy-jejunostomy tube) if they aren’t ready to start eating and drinking by mouth.
- Your child’s team, with the help of the feeding team, will decide if/when your child is ready to start eating or drinking.
When can I hold my child and when can they move around?
- After the first trach change, your child can begin to move with help from a physical therapist (PT) if they’re stable.
- Depending on your child’s age, PT will work on your child’s gross motor skill development, strength, independent play and mobility.
- Babies are able to participate in tummy time with some modifications, with permission from the medical team. PT and occupation therapy (OT) can help you and your baby learn how to safely do tummy time with a trach.
Who will help me get the equipment and supplies I need at home?
- A nurse case manager will meet with you and the team to review your discharge (leaving the hospital) needs. This includes transferring to rehab or going home, your child’s care needs, equipment, supplies and home nursing.
- They will work with your insurance and outside home vendors (suppliers) to coordinate what you need after you leave.
How can I help my child emotionally?
- Child Life specialists are people who are trained to help support families as they go through medical procedures and changes.
- They have developmentally appropriate resources to support your child and your family.
- Your nurse/team can help you contact a Child Life specialist.
Who do I call if I have a problem with my child’s trach after we go home?
- Call 911 if there is an emergency.
- If you have a non-urgent question, call the doctor who is caring for your child in your community (pediatrician).
- You will have follow up with ORL in the Tracheostomy clinic or Otolaryngology clinic, the clinic staff will reach out to set up an appointment. If your child needs a ventilator at home, they may be followed by a pulmonologist or the CAPE Team (a service for children with chronic respiratory insufficiency, technology dependence and related medical complexities).
- You will meet the team that will help you at home before you leave the hospital.
